What Is A Herniated Disc?
The lower backbone called the lumbar spine is made up of bones called vertebrae that stack up against one on top of the other. In between the vertebrae is a cartilage called a disc that acts as a cushion and allows your spine to bend in a different direction. The disc has layers, like an onion, called the annulus fibrosus, and a gel-like center called the nucleus pulposus. The disc also contains high content of water.
With age, the water content in the disc reduces and loses its ability to act as a cushion. This may predispose a displacement of the disc’s center (called a herniated or ruptured disc) through a crack in the outer layer.
Causes
The most common causes are repetitive injuries, micro or major trauma, heavy lifting, pushing, pulling activities, and degenerative changes to the disc annulus.
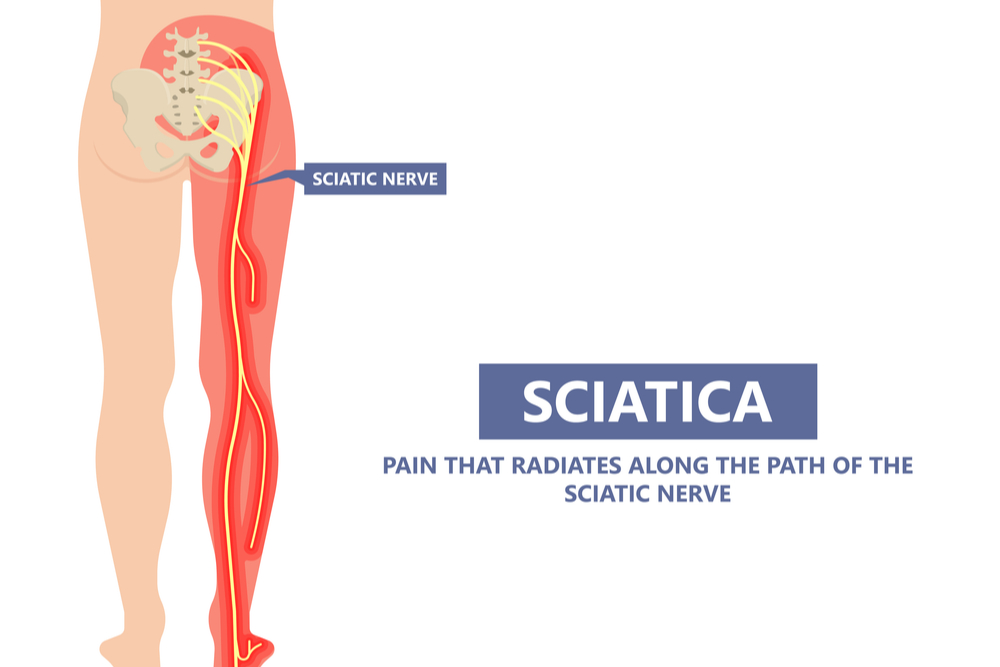
A herniated lumbar disc may also cause back pain which can travel down the leg, although back pain alone (without leg pain) can have many causes other than a herniated disc.
Risk Factors
Smoking, age (30-55), height (taller), sex (males) heavy work are associated with increased risk.
Signs and Symptoms
When a disc herniates it can irritate, inflame or compress a nerve (pinched nerve) that causes the most pain, and sometimes numbness, tingling, or weakness in the back that travels down the legs, known as sciatica which can also be associated with pain in the legs.
Screening & Diagnosing
A complete history and physical with laboratory testing are done which can identify the diagnosis, causes, and future treatment options. Back or neck pain & or Sciatica can have many other causes of pain other than a herniated disc.
An X-ray, CT scan, and/or MRI of the lumbar spine may be indicated. A detailed MRI is most accurate in evaluating herniated discs. Often an MRI may not be indicated if symptoms are mild and active treatment can resolve symptoms. If symptoms of nerve root involvement are present for over six weeks an Electromyogram (EMG) and Nerve conduction study (NCS) can be performed. It involves using electric stimulation of nerves & a tiny needle electrode in the resting and contracting muscles supplied by affected nerves. This test can determine the extent & level of actual nerve damage.
Epidural steroid injections: As a herniated disc may leak chemicals or irritate the nerves, epidural steroid injections may be necessary in severe cases or after physical therapy and medications have failed to provide pain relief. These injections (discussed in another pamphlet) are done at our practice using fluoroscopic (x-ray guidance) using advanced techniques in Interventional pain management (discussed more in another pamphlet). Potent steroids are placed at the interface of the pain source to help reduce pain and inflammation around the nerve and disc that is causing the pain in the back and to travel down the buttock or leg. It can therefore give the body a chance to heal and recover from the condition, continue with further rehabilitation and avoid surgery. It is our practice to treat pain aggressively and early (3-6 months of pain onset) to try to get to the source of pain rather than masking the pain with narcotic medications or prolonged passive physical therapy. This is important in avoiding chronic pain, disability, disuse, dependency on drugs, and emotional anxiety/depression related to pain.

